Telemedicine for Diabetes India: 7 Revolutionary Changes
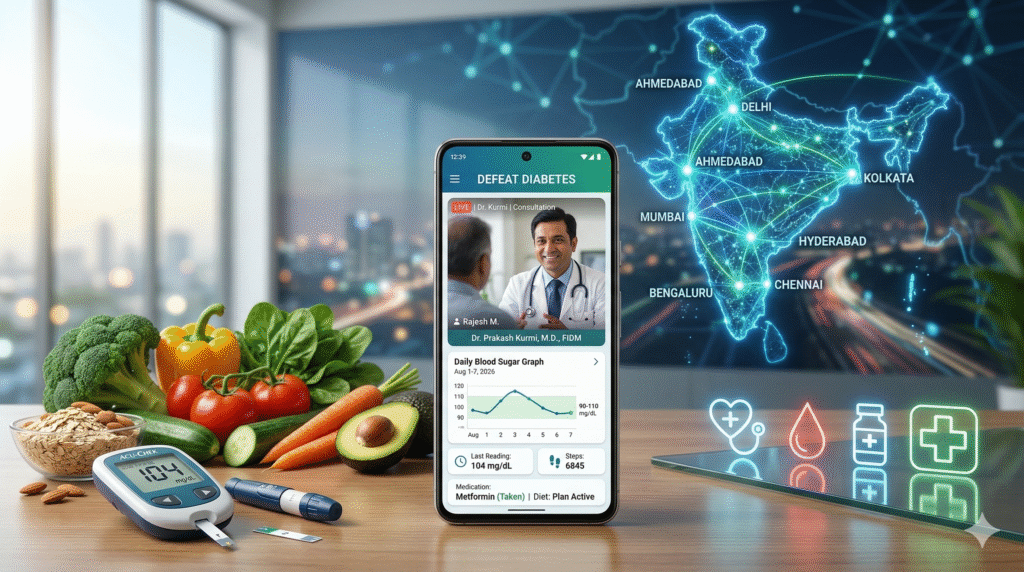
Home › Blogs › Telemedicine for Diabetes in India 🔥 TRENDING: How Digital Healthcare is Revolutionizing Diabetes Management in India | Last Updated: March 10, 2026 Telemedicine for Diabetes in India: How Defeat Diabetese is Leading the Digital Health Revolution Telemedicine for diabetes in India has emerged as a game-changing solution to the nation’s healthcare challenges, and Defeat Diabetese stands at the forefront of this transformation. With over 101 million Indians living with diabetes and traditional healthcare infrastructure struggling to meet demand, telemedicine for diabetes in India offers unprecedented access to expert care. This comprehensive analysis explores how digital healthcare is revolutionizing diabetes management, why Defeat Diabetese represents the future of metabolic health in India, and the massive opportunity this presents for patients, doctors, and healthcare innovation. From AI-powered glucose tracking to remote consultations with leading diabetologists, discover how telemedicine for diabetes in India is saving lives and transforming outcomes. 📊 The Diabetes Crisis in India (2026) 101M+ Indians with Diabetes 136M+ Pre-Diabetics 75% Skip Follow-ups 1:100K Doctor-Patient Ratio Table of Contents The Rise of Telemedicine for Diabetes in India India’s Diabetes Epidemic: The Numbers Behind the Crisis Why Traditional Diabetes Care is Failing How Telemedicine Solves Core Healthcare Problems Defeat Diabetese: The Startup Revolutionizing Diabetes Care DefeatDM App: Technology Powering Transformation Real Patient Outcomes: Data from 100,000+ Cases Sustainable Business Model: Making Healthcare Affordable The $10 Billion Opportunity in Diabetes Telemedicine Government Initiatives Supporting Digital Health Vision 2030: Transforming 10 Million Lives How Patients Access Defeat Diabetese Telemedicine Building India’s Largest Diabetes Doctor Network Frequently Asked Questions The Explosive Rise of Telemedicine for Diabetes in India Telemedicine for diabetes in India isn’t just a trend—it’s a fundamental transformation of healthcare delivery driven by necessity, technology, and changing patient expectations. The COVID-19 pandemic accelerated adoption by nearly 5 years, proving that remote healthcare could deliver outcomes equal to or better than traditional care. Market Growth & Adoption Statistics 📈 India’s Telemedicine Market Trajectory 2020: $830 million market size (pre-pandemic baseline) 2023: $5.4 billion (550% growth post-COVID) 2026 (Current): $11.2 billion estimated 2030 (Projected): $30+ billion at 28% CAGR Diabetes segment: Represents 23% of total telemedicine consultations What makes telemedicine for diabetes in India particularly compelling is its alignment with the chronic nature of the disease. Unlike acute conditions requiring emergency intervention, diabetes demands continuous monitoring, frequent medication adjustments, lifestyle counseling, and long-term relationship with healthcare providers—all perfectly suited to digital delivery. Key Drivers of Telemedicine Adoption Driver Impact on Diabetes Care Smartphone Penetration 750M+ smartphone users; 4G/5G connectivity in Tier 2/3 cities enables video consultations Digital Literacy UPI adoption proved Indians embrace digital services; healthcare naturally follows Specialist Shortage Only ~25,000 endocrinologists for 101M diabetics; telemedicine bridges gap Urban Migration Families separated geographically; telemedicine enables care for aging parents Cost Pressure 60% medical expenses out-of-pocket; telemedicine reduces travel, time, total costs India’s Diabetes Epidemic: Understanding the Scale of the Crisis Before exploring how telemedicine for diabetes in India provides solutions, we must understand the magnitude of the problem. India has earned the unfortunate title of “Diabetes Capital of the World”—and the numbers paint a sobering picture. The Diabetes Burden in Numbers ⚠️ Critical Statistics (2026 Data) 101.2 million adults living with diabetes (ages 20-79) 136 million people with pre-diabetes (impaired glucose tolerance) 1 in 3 adults has either diabetes or pre-diabetes 57% undiagnosed: Over 57 million Indians have diabetes but don’t know it Economic burden: ₹97,000 crores annually in direct medical costs Productivity loss: ₹1.2 lakh crores due to diabetes-related absenteeism and disability Life expectancy impact: Diabetes reduces lifespan by 8-10 years if poorly controlled Why India? Understanding the Risk Factors Indians develop diabetes at younger ages (onset 10-15 years earlier than Europeans) and at lower BMI levels. This “Asian Indian Phenotype” combines genetic predisposition with rapid lifestyle changes: Genetic susceptibility: Indians have higher visceral fat accumulation even at normal weight Rapid urbanization: Shift from agricultural to sedentary work (70% urban population by 2030) Dietary transition: Traditional balanced diets replaced by processed foods, refined carbs Economic growth paradox: Rising incomes enable calorie-dense diets without corresponding health awareness Stress epidemic: Competitive work culture, nuclear families, financial pressures Poor healthcare infrastructure: Inadequate prevention programs, late diagnosis Why Traditional Diabetes Care is Failing Millions of Indians Despite growing awareness, conventional healthcare delivery models struggle to meet the diabetes challenge. Understanding these failures reveals why telemedicine for diabetes in India isn’t optional—it’s essential. The 7 Critical Failures of Traditional Diabetes Care ❌ Problem 1: Specialist Shortage The Gap: Only ~25,000 endocrinologists and diabetologists for 101 million patients (1:4,000 ratio). Recommended ratio: 1:500. Most specialists concentrated in metros, leaving Tier 2/3 cities underserved. ❌ Problem 2: Follow-up Failure The Reality: 75% of patients skip recommended follow-ups due to distance, time constraints, work schedules, or transportation costs. Diabetes requires quarterly monitoring minimum—most patients see doctors only when crises occur. ❌ Problem 3: Medication Non-Adherence The Numbers: Only 43% of diagnosed diabetics take medications regularly. Reasons include cost (30% medication budget), complex regimens, side effects, and lack of continuous guidance on adjustments. ❌ Problem 4: Fragmented Care The Problem: Patients see multiple providers (GP, endocrinologist, ophthalmologist, nephrologist, cardiologist) with no coordination. Medical records scattered across clinics. No single provider owns the complete care journey. ❌ Problem 5: Inadequate Lifestyle Support The Gap: Doctors spend 80% of 15-minute consultations on medication, leaving minimal time for critical lifestyle counseling. Patients receive generic diet sheets instead of personalized, culturally adapted plans. ❌ Problem 6: High Out-of-Pocket Costs The Burden: Average annual diabetes cost: ₹38,000-₹1,20,000 (consultations + medications + tests + complications). With 60% healthcare spending out-of-pocket, families make impossible choices between treatment and other needs. ❌ Problem 7: Late Diagnosis The Crisis: 57% discover diabetes only when complications appear (vision problems, kidney disease, neuropathy). By then, reversing damage becomes difficult. Lack of routine screening in primary care means missed opportunities for early intervention. How Telemedicine for Diabetes in India Solves Core Healthcare Problems Telemedicine for diabetes in India doesn’t just digitize existing care—it fundamentally redesigns the patient experience to
Telemedicine for Diabetes India: 7 Revolutionary Changes Read More »